The things we do for safety: Battling bacteria (part 1)
Wednesday, February 08, 2017 Dr. Sophie Chargé
A previous post in our "The things we do for safety" series explores leukoreduction - or how white blood cells or leukocytes get filtered out of blood products to reduce the risk of transfusion-related reactions.
Battling bacteria (part 1)
Bacteria can be found pretty much everywhere and while some contribute to our wellness others can cause serious harm, especially if transfused to a patient whose health is already compromised. Over the years, blood operators have implemented a variety of measures to limit the bacterial contamination of blood components. In this series on “Battling bacteria”, we will explore the measures we take to keep bacteria out of blood products and enhance the safety of the blood system.
One possible source of contamination is the bacteria that normally live on the skin. Human skin is home to millions of microorganisms. Skin microflora includes many different types of bacteria, which may enter the collected blood during the donation process. If bacteria are collected along with the blood donation, some may survive and even thrive during storage.
Therefore, our first line of defense against bacterial contamination is to thoroughly disinfect the arm of the donor — we call this the arm scrub. When suppliers change the products we use for the disinfection, like in 2015, we conduct research to make sure the new disinfectant will be as effective. So that is why, before every donation, the nurse will thoroughly scrub your arm!
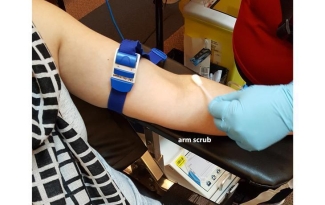
While the arm scrub is effective at eliminating some bacteria, it is not sufficient all by itself. In fact our own researchers have shown that some bacteria are resistant to the bactericidal action of disinfectants.
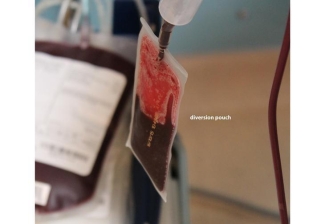
A second line of defense is to divert the first few millilitres of the donation to a diversion pouch. Included in the first few millilitres is the “skin plug” — the bit of skin pushed through by the needle — to which the bacteria are attached.
Another source of bacterial contamination could be from the donor blood. Donors are asked a number of questions prior to their donations. A few of those questions are aimed at assessing whether the donor may have an extra risk of having bacteria in their blood. Fever, piercings, tattoos and dental visits are among the questions asked that reflect this additional risk. If indeed a donor identifies such risk, they will be asked to donate at a later date when that risk has passed.
In part 2 of The things we do for safety: Battling bacteria, we will tell you about the other lines of defense we put in place to reduce bacterial contamination of blood products to ensure their safety for Canadian patients.
Further reading
Dr. Sandra Ramirez, a development scientist at Canadian Blood Services’ Center for Innovation in Ottawa, is our in-house microbiology expert. Discover a few recent projects aimed at improving safety and quality of blood products.
- ResearchUnit: Dodging disinfection: biofilm-forming skin bacteria can resist disinfectants.
- Video: Challenging the 30 minute rule
A previous post in our "The things we do for safety" series explored leukoreduction — how white blood cells or leukocytes get filtered out of blood products to reduce the risk of transfusion-related reactions.
Canadian Blood Services – Driving world-class innovation
Through discovery, development and applied research, Canadian Blood Services drives world-class innovation in blood transfusion, cellular therapy and transplantation—bringing clarity and insight to an increasingly complex healthcare future. Our dedicated research team and extended network of partners engage in exploratory and applied research to create new knowledge, inform and enhance best practices, contribute to the development of new services and technologies, and build capacity through training and collaboration. Find out more about our research impact.
The opinions reflected in this post are those of the author and do not necessarily reflect the opinions of Canadian Blood Services nor do they reflect the views of Health Canada or any other funding agency.
Related blog posts
Led by Dr. Sandra Ramirez, a development scientist at Canadian Blood Services’ Centre for Innovation, this research project led to a new standard that will reduce the number of discarded red blood cell units. By Jenny Ryan and Patrick Walton The issue Since the 1970s, blood operators have limited...
Canadian Blood Services implemented leukoreduction for the production of its red blood cells and platelet components in the late 1990s.

